Celebrities and their eyes have been in the news a lot recently. Both Taylor Swift and Kylie Jenner have gotten LASIK in the last month! But what you may have missed was something that happened back in April.
This is when Warriors star Stephen Curry admitted he has a vision disease. The culprit? An eye condition called keratoconus. Haven’t you heard of it? Keep reading to learn more about this eye condition!
Did Keratoconus Hurt Steph Curry’s Game?
How can one of the NBA’s best players have a serious eye condition and still shoot three-pointers effortlessly? Back in April at a press conference, Curry revealed he had upped his game thanks to special contact lenses.
Now, these aren’t the normal contacts that you wear for a month and then dispose of. Instead, when you have keratoconus, you’ll usually wear gas permeable contact lenses, if you can wear contacts.
GP lenses are harder than a soft contact lens and help replace the cornea’s irregular shape that keratoconus causes. Thanks to his new contact lenses, Curry no longer experiences blurry vision, squinting, or visual discomfort while dominating on the court!
What Is Keratoconus?
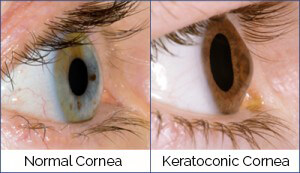
Keratoconus is an eye condition that affects millions of people around the world. In a normal eye, the cornea is a dome-shaped window that focuses light into the eye.
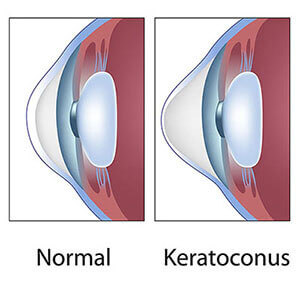
When you have keratoconus, the cornea gets thinner and bulges out, resembling a cone. As the shape of the cornea changes, light rays coming into the eye are out of focus.
This results in blurry and distorted vision. For people with keratoconus, this makes ordinary tasks more difficult than they should be.
What Causes Keratoconus?
Doctors aren’t 100% sure what causes keratoconus. It does seem to have some genetic qualities, where it is passed down through family members.
For about 1 in 10 people with keratoconus, they have a parent who also has it. There is also an association with excessive eye rubbing and eye allergies and those with keratoconus.
In most cases, keratoconus starts in the late teens to the early twenties. Once diagnosed, vision will slowly get worse over ten to twenty years.
What Are The Most Common Symptoms Of Keratoconus?
For many people with keratoconus, it affects both eyes. If you have keratoconus in both eyes, it can lead to drastically different vision between eyes.
Early symptoms of keratoconus may include slightly blurry vision, a distorted vision where lines look wavy, more sensitivity to light or glare, redness, and swelling.

As keratoconus progresses, symptoms and visual distortion continue getting worse. This will usually mean you have increased astigmatism or nearsightedness.
If you experience this, your eyes won’t focus as well as they used to be able to. Patients with more advanced stages of keratoconus will need new glasses prescriptions on a more frequent basis.
You may also find it too difficult to wear contact lenses anymore. This is because of the bulging shape of the cornea. Contact lenses won’t fit and will probably become very uncomfortable to wear.
How Can You Treat Keratoconus?
There are several ways you can treat the symptoms of keratoconus. How you treat keratoconus depends on the severity of your symptoms and what stage of the condition you are in.
Beginning Stages: Eyeglasses
If you are diagnosed in the beginning stages, you can usually start with wearing eyeglasses. As your vision continues worsening, there are other treatments you can try.
Gas Permeable Contact Lenses
Like Stephen Curry, you may try using gas permeable contact lenses to treat your keratoconus. If you do, expect to visit your eye doctor for frequent visits.
This is to ensure both fit and your prescription are accurate. Both are bound to change frequently as your keratoconus continues progressing.
Intacs
Another option you may try is Intacs. Intacs are clear, arc-shaped corneal inserts that are FDA approved. They are surgically inserted within the peripheral cornea.
This lets them reshape the front surface of the eye to achieve a clearer vision. Intacs may become necessary if you can no longer correct your vision using contact lenses or glasses.
Corneal Cross-Linking
At Chicago Cornea Consultants™, Ltd. we offer keratoconus patients several options. One is Corneal Cross-Linking (CXL).
CXL takes Riboflavin, which is a Vitamin B derivative, and UV light to create cross-links between the cornea’s collagen fibers. By creating these cross-links, it makes the cornea more rigid and prevents further changes from developing.
There are two forms of CXL available: epithelium-ON and epithelium-off. Although we offer both techniques to our patients, there are fewer risks with the epithelium-off technique. There is also a decreased risk of scarring, infection, and less discomfort.
With CXL, patients will still need to wear glasses or contacts to correct their vision after receiving the procedure. The goal with CXL is to preserve existing vision and prevent further vision loss.
Advanced Stages: Corneal Transplant Surgery
Another treatment option that Chicago Cornea Consultants™, Ltd. offers keratoconus patients is a cornea transplant. For advanced stages of keratoconus, a cornea transplant may become necessary.
If the cornea is too damaged, the unhealthy cornea is replaced with a healthy cornea donated to an eye bank. The damaged cornea is carefully removed, and the clear donor cornea is then sewn into place.
Once the donor cornea has been securely sewn on, a shield is then placed over the eye to protect it. Even after a cornea transplant, it’s likely that you’ll still need glasses or contacts to see clearly.
Concerned that you may have keratoconus? Schedule an appointment at Chicago Cornea Consultants™, Ltd. in Chicago, IL now!

